When to See a Fertility Therapist (Not Just a Fertility Clinic)
When to See a Fertility Therapist (Not Just a Fertility Clinic)
Your fertility clinic monitors your hormones. They track your follicles, measure your lining, adjust your medications, and time your procedures down to the hour.
What they don't monitor: how you're actually doing.
Fertility treatment is medically intensive. It's also emotionally intensive. And while clinics are equipped for one, they're rarely equipped for the other.
That's where a fertility therapist comes in. Not as a replacement for medical care, but as an essential complement to it.
The gap between medical care and emotional support
Fertility clinics are built for efficiency. Appointments are short. Protocols are standardized. Your reproductive endocrinologist is an expert at getting you pregnant, not at helping you cope with the emotional weight of trying.
Most clinics offer some form of counseling, often a social worker or psychologist available for mandated sessions before egg donation, surrogacy, or other third-party reproduction. But these are typically brief, protocol-driven appointments designed to satisfy clinical requirements, not to provide ongoing therapeutic support.
The gap matters. Research in Dialogues in Clinical Neuroscience found that 25 to 60 percent of infertile individuals report psychiatric symptoms, with anxiety and depression levels significantly higher than in fertile controls. Yet despite these high rates, very few patients seek or receive psychiatric care. One study noted only 6.7 percent of infertility patients accessed mental health support.
This disconnect has real consequences. Research shows that psychological distress is the most frequent cause of treatment discontinuation in insured patients. People don't stop treatment because they can't afford it or because their prognosis is poor. They stop because they're emotionally depleted.
What a fertility therapist actually does
A fertility therapist is a mental health professional with specialized training in reproductive mental health. We understand the medical landscape, the IVF protocols, the medication side effects, the two-week wait, the beta call, but our focus is on helping you navigate the psychological experience of it all.
This isn't general talk therapy. Fertility therapy is targeted, informed support for the specific challenges of trying to conceive:
Processing cumulative loss. Negative pregnancy tests, failed cycles, miscarriages. The losses accumulate. A fertility therapist helps you grieve without getting stuck in grief.
Managing fertility-specific anxiety. The hypervigilance. The symptom-spotting. The catastrophizing. The intrusive thoughts about what might go wrong. We help you interrupt these patterns using evidence-based approaches.
Navigating medication effects. Clomiphene, leuprolide, and gonadotropins are all associated with psychological symptoms including anxiety, depression, and irritability. It's hard to distinguish between emotional responses to infertility and medication side effects. A fertility therapist can help you sort through this.
Supporting decision-making. When to keep going. When to take a break. Whether to try a different protocol, change clinics, or consider donor eggs, surrogacy, or adoption. These decisions are emotional, not just medical, and benefit from therapeutic support.
Protecting your identity. Many people lose themselves in treatment. Therapy helps you maintain a sense of who you are beyond your fertility status.
Addressing relationship strain. Infertility affects couples. We help partners communicate, stay connected, and navigate treatment as a team.
The research on psychological intervention in fertility
The evidence supports what fertility patients often intuitively know: mental health matters.
A comprehensive review published in Dialogues in Clinical Neuroscience found that psychological interventions, especially those emphasizing stress management and coping-skills training, have beneficial effects for infertility patients. The researchers noted that addressing psychological symptoms may help reduce treatment dropout and potentially improve outcomes.
A meta-analysis including 39 studies found that psychosocial interventions reduce negative affect in fertility patients. Some studies also found improvements in pregnancy rates, though results were mixed. The researchers concluded that interventions lasting six or more sessions were more impactful than shorter ones.
One particularly noteworthy finding: A study measuring hair cortisol (which reflects stress levels over the prior three to six months) found that cortisol levels were significantly correlated with pregnancy rates. Women with lower stress had better outcomes.
This doesn't mean you should feel pressure to "relax," a piece of advice that's both unhelpful and often harmful. It means that your mental health deserves attention and support as part of your fertility care, not as an afterthought.
Signs you might benefit from a fertility therapist
You don't need to be in crisis to seek support. Consider reaching out if:
You're having trouble sleeping, eating, or concentrating because of fertility stress
You dread treatment appointments or feel numb during the process
You've experienced pregnancy loss and are struggling to try again
You and your partner are arguing more, feeling distant, or coping very differently
You feel like you've lost yourself in the fertility journey
You're questioning whether to continue treatment and need help processing the decision
You're experiencing symptoms of anxiety or depression that feel unmanageable
You've had thoughts about self-harm (research shows 9.4 percent of women with infertility report suicidal thoughts or attempts)
What to look for in a fertility therapist
Not all therapists have training in reproductive mental health. When searching for support, look for someone who:
Has specific experience with infertility, IVF, pregnancy loss, and family-building. Ask directly about their background and training.
Understands the medical terminology and treatment protocols. You shouldn't have to spend session time explaining what an IUI is or how a retrieval works.
Won't offer toxic positivity. "Just relax" and "it will happen when it's meant to" are not therapeutic interventions. Look for someone who can sit with uncertainty and difficult emotions.
Offers flexible scheduling. Fertility treatment is unpredictable. You need a therapist who can accommodate last-minute changes.
Uses evidence-based approaches. Cognitive behavioural therapy (CBT), interpersonal therapy (IPT), acceptance and commitment therapy (ACT), and mindfulness-based interventions all have evidence supporting their use in fertility-related distress.
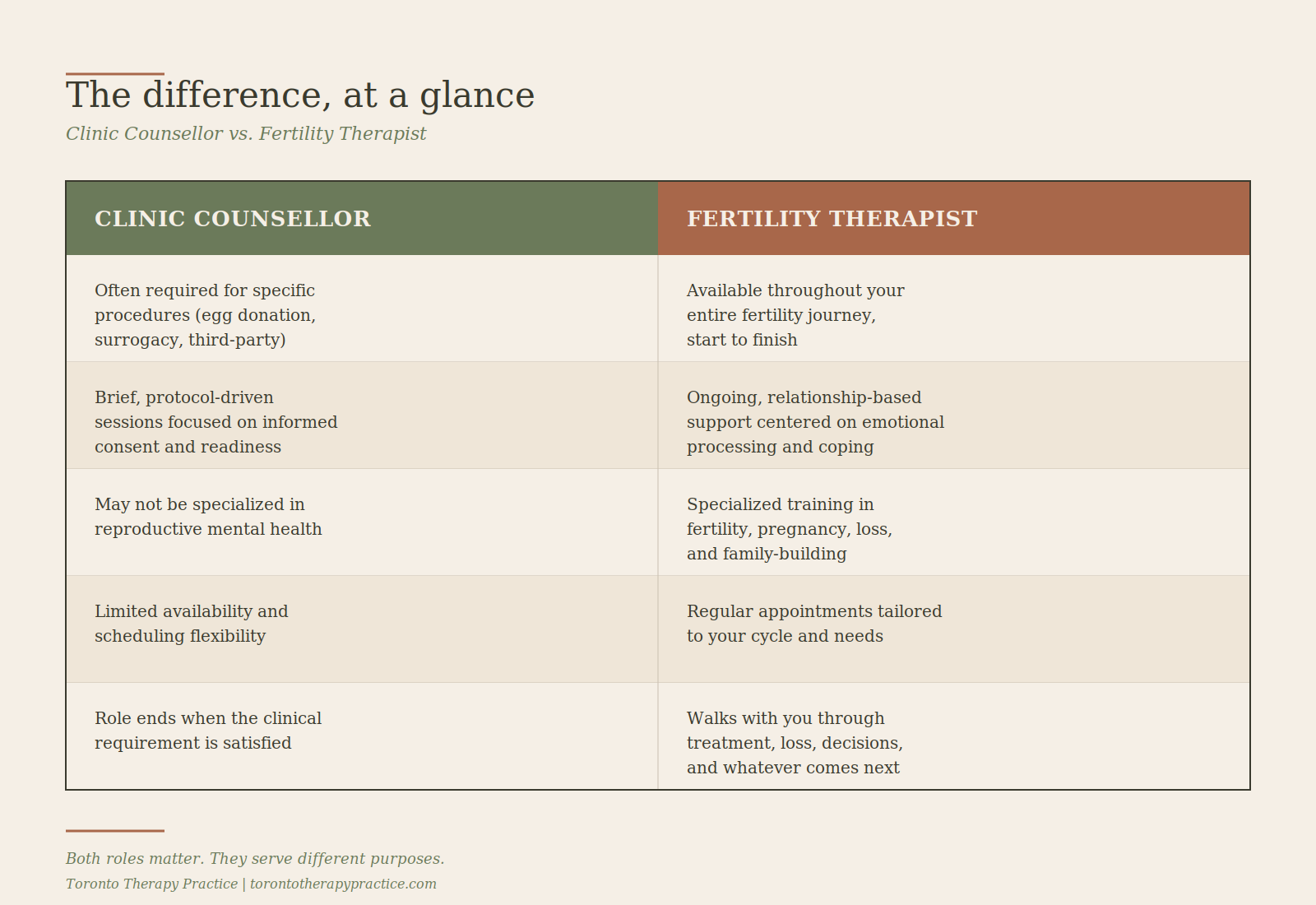
The difference between a fertility therapist and a clinic counselor
Clinic counsellors serve an important function, but their role is different from ongoing fertility therapy.
Both have value. But if you're looking for sustained emotional support through fertility treatment, a dedicated fertility therapist is what you need.
At Toronto Therapy Practice
Our team includes therapists who have worked in hospital-based reproductive mental health programs, including the Mount Sinai Mother-Baby Unit and Special Pregnancy Program. We understand fertility treatment from the inside.
We offer:
Individual therapy for anyone navigating fertility challenges
Couples therapy to help partners stay connected through treatment
Support for pregnancy after loss, LGBTQ+ family-building, and third-party reproduction
Flexible scheduling that accommodates treatment cycles
Your fertility clinic is tracking your body. Let us help you take care of your mind.